- Heavy or prolonged menstrual bleeding
- Pelvic pain or pressure
- Frequent urination
- Pain during intercourse
Uterine fibroids are common, but living with the pain, heavy bleeding, and disruption they cause doesn’t have to be. At Endovascular Consultants of Delaware, we offer Uterine Fibroid Embolization (UFE)—a minimally invasive treatment that shrinks fibroids, relieves symptoms, and helps you get back to living your life.
Fibroids are non-cancerous growths that develop in or around the uterus. While they aren’t life-threatening, they can have a major impact on your quality of life.
If you’re experiencing these symptoms, you're not alone—and you have options beyond major surgery.
UFE is a minimally invasive procedure that blocks the blood supply to fibroids, causing them to shrink and symptoms to improve. It’s performed by an interventional radiologist and usually takes under an hour.
UFE has a 90%+ patient satisfaction rate and is often an alternative to hysterectomy or myomectomy.
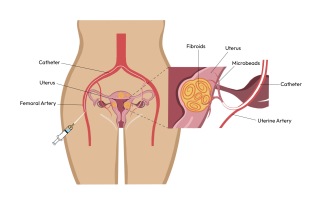
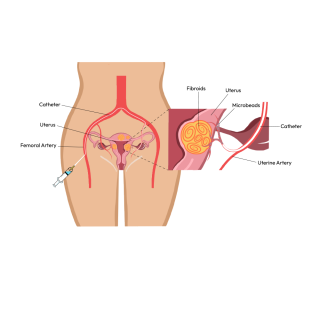

At EVC, we empower women to make informed, confident decisions about their health.
Every treatment plan is personalized based on your health, risk factors, and goals.
Many women are only presented with surgical options like hysterectomy—but there are alternatives. As interventional radiologists, we treat fibroids with small incisions, image guidance, and faster recovery.
Before you commit to surgery, find out if UFE could be right for you.
You don't have to live like this. Let's explore your options together.

Dr. Mark J. Garcia is a board-certified, world-renowned interventional radiologist with over 25 years of experience. He has held leadership positions across some of the nation’s top vascular centers and medical device companies. Known for his pioneering work in minimally invasive treatments, Dr. Garcia is committed to improving outcomes for every patient he meets.